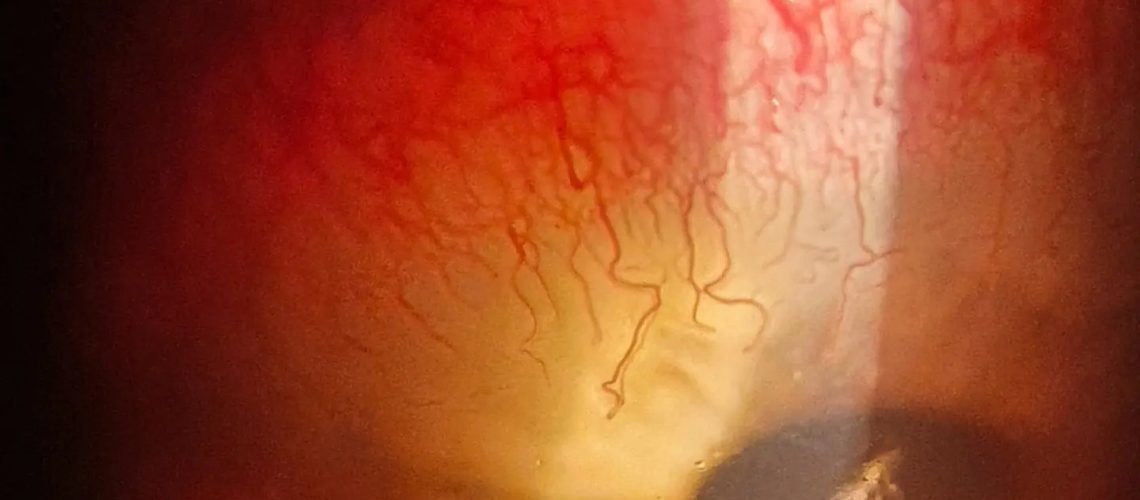
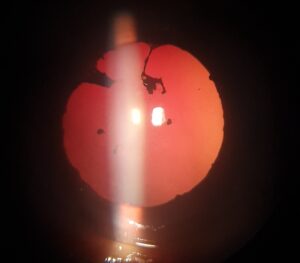
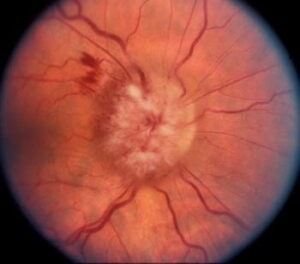
is a vision-threatening condition that introduces delicate blood vessels into the normally avascular cornea (meaning it has no blood vessels), that can extend from the limbus into the superficial or deep areas of the cornea, which compromises its transparency.
This can be caused by inflammation related to infection, chemical injury, autoimmune conditions, immune hypersensitivity, post-corneal transplantation, and traumatic conditions, contact lens complications among other ocular pathologies. Immature new blood vessels may lead to lipid exudation, persistent inflammation, and scarring, thus threatening corneal transparency and visual acuity.
Most corneal neovascularization is the result of extended contact lens wear that is compromising the amount of oxygen getting to the cornea. Early contact lens wear related corneal neovascularization usually presents as a superficial pannus, commonly at the superior limbus, under the upper lid. As this is likely related to hypoxia.
Hypoxia occurs when the cornea does not get enough oxygen. It is the most common complication of contact lens wear, especially extended-wear lenses. The cornea has no blood supply of its own, so it gets oxygen only from tears and directly from the atmosphere.
Physiologically, it is known that hypoxia causes cells to release inflammatory cytokines which can induce new vascular growth. This is as true in the cornea as it is in the retina. When the cornea is deprived of enough oxygen the endothelium pump loses efficiency and is unable to maintain the relatively dehydrated state of the corneal tissue, and therefore it begins to swell. When the decrease in available oxygen becomes chronic, the cornea responds by allowing tiny new blood vessels to grow. This is corneal neovascularization.
Occasionally toric hydrogel contact lenses can also elicit such a pannus but at the lower limbus, where these lenses are thickest by design. The wear of GP CLs has minimal risk of causing neovascularization but might, if of low oxygen permeability.
The treatment of corneal neovascularization is problematic. However, a variety of off-lab treatment approaches, such as topical treatments, have been shown to produce varying degrees of effectiveness.
Many patients can be helped by just decreasing wear from extended to daily use, and perhaps increasing the oxygen permeability of the lenses they use, refitting from a hydrogel to a silicone hydrogel contact lens.
If vision dysfunction is severe, and especially if due to lipid deposition in the corneal apex, unfortunately, it is most likely that the patient will require a corneal transplant, perhaps lamellar or penetrating, to restore vision.
The final clinical maneuver would be to discontinue CL wear.
People who are at risk for CN are
- Contact lens wearers, especially those who are non-compliant with lens care
- People who have large amounts of nearsightedness (myopia)
- Sufferers of dry eye disease
- Those who have an ocular surface disease (rosacea, lupus)
- Those who have an underlying inflammatory disease (multiple sclerosis, Crohn’s Disease)
- Those with untreated, or inadequately treated, infection of any ocular tissues
Prognosis
Once blood vessels have grown into the corneal tissue, they will not disappear completely. By increasing the oxygen getting to the cornea, it is possible to stop their growth, but the best result will still leave ghost vessels there. If at any time, the cornea is again compromised for lack of oxygen, those vessels will fill up and begin to grow again.