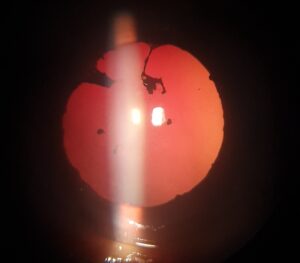
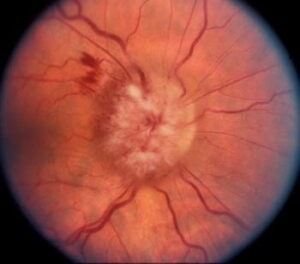
Uveitis is an inflammation of the uvea, which is the central layer of the eye sandwiched between the iris, the choroid and the ciliary body. It’s a potentially life-threatening illness that, if untreated, can cause blindness.
People of all ages, including youngsters, are susceptible to developing the illness, which can damage either one or both eyes.
It can be called acute or chronic anterior uveitis based on how it affects the patient, granulomatous or non-granulomatous anterior uveitis based on how it looks, or infectious or non-infectious anterior uveitis based on what caused it.
Causes: Uveitis can be caused by various factors, including:
- Autoimmune disorders (rheumatoid arthritis, lupus, sarcoidosis)
- Infections (bacterial, viral, fungal, or parasitic)
- Injury or trauma to the eye
- Certain medications
- Genetic predisposition
- Smoking
Symptoms
In some situations, symptoms grow gradually over time, while in others, they appear suddenly and rapidly worsen. Uveitis symptoms and characteristics can include the following.
- Eye redness.
- Eye pain.
- Light sensitivity.
- Blurred vision.
- Dark, floating spots in your field of vision (floaters).
- Decreased vision.
Uveitis can be dangerous and can vary in intensity from mild to severe based on a number of factors, including the underlying cause, the degree of inflammation, and the speed with which it is treated. Uveitis can cause glaucoma, cataracts, retinal detachment, and even permanent vision loss if it is not treated or is treated inadequately.
Types of Uveitis:
Uveitis can be classified into several types based on the part of the uvea that is affected:
- Anterior uveitis: Inflammation primarily affecting the front of the eye, including the iris and ciliary body.
- Intermediate uveitis: Inflammation affecting the middle portion of the eye, including the vitreous gel.
- Posterior uveitis: Inflammation affecting the back of the eye, including the choroid and retina.
- Panuveitis: Inflammation involving all parts of the uvea.
Treatments
The goal of treating uveitis is to decrease inflammation, ease symptoms, and avoid further problems. The severity of the uveitis and its etiology will determine the best course of treatment. Examples of typical methods of treatment are:
- Inflammation in the eye can be reduced with the help of topical or oral corticosteroids.
- Immunosuppressive medications: These may be used when the condition is severe, or when corticosteroids alone are not enough to control the immune response.
- Pain relievers and inflammatory medication options include nonsteroidal anti-inflammatory medicines (NSAIDs).
- Newer medications called “biologic agents” may be utilized in some situations since they target specific parts of the immune system.
- Cataract and retinal detachment are two consequences of uveitis that may require surgical intervention for treatment.
Prevention
Uveitis may not always be avoidable, however the following steps may help lessen the likelihood of it happening or the degree to which it does:
- Routine eye exams: Uveitis can be detected and treated quickly if they are performed routinely.
- The risk of uveitis can be lowered by treating the underlying problems that cause it, including as autoimmune diseases or infections.
- Preventing eye injuries that could lead to uveitis is as simple as wearing protective eyewear like goggles or safety glasses whenever possible.
- A balanced diet, frequent exercise, and plenty of sleep all contribute to a healthy lifestyle, which in turn may benefit your eyes.