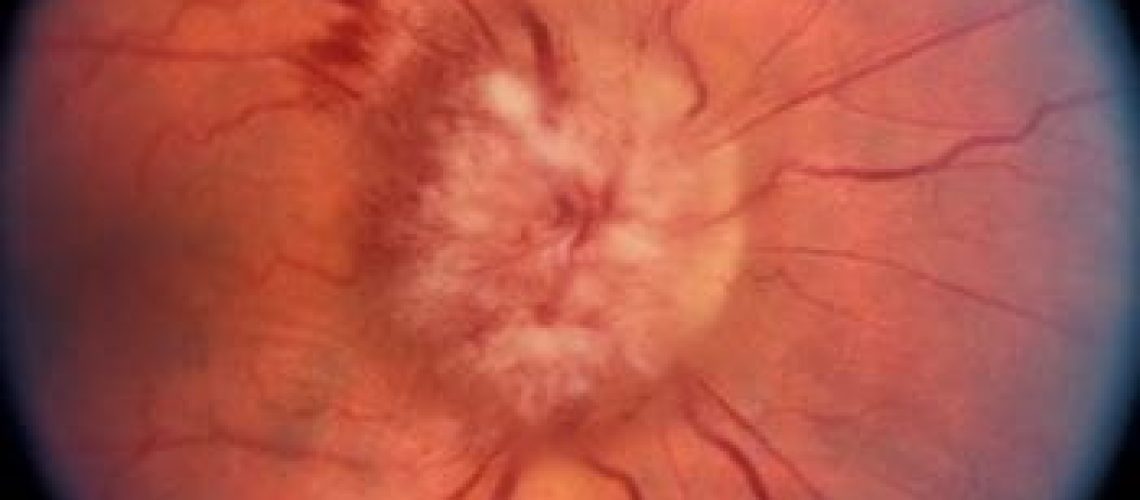
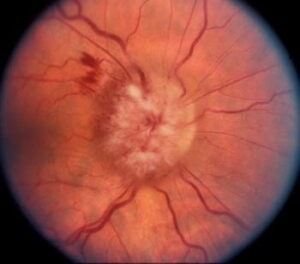
Papilledema is a medical condition in which the optic nerve head (or optic disk) is swollen due to increased pressure within the skull. This condition is a serious sign of an underlying medical problem and can lead to permanent vision loss depending on the severity and if not treated promptly.
Fundus examination reveales edema of the optic disc. Opacification of the retinal nerve fibers, elevation of the margins, hyperemia and obliteration of the cup, venous dilation, vascular tortuosity, hemorrhages, cotton-wool spots and exudates that may extend to the macula causing a macular star appearance.
The time course for the development of papilledema can be weeks if there is only a slow and mild increase in intracranial pressure, but severe and rapid changes in pressure can cause papilledema to appear within a few hours or a day. .
Papilledema’s Causes
The most common cause of papilledema is increased pressure within the skull, also known as intracranial pressure. This can be caused by a number of factors including:
- Brain tumors
- Idiopathic intracranial hypertension (IIH), a condition characterized by high pressure within the skull with no obvious cause.
- Hydrocephalus, a condition in which there is an accumulation of cerebrospinal fluid (CSF) within the skull.
- Infections such as meningitis or encephalitis.
- Traumatic brain injury.
- Blood clots within the brain.
- Chronic sinusitis or other infections.
- Malignant hypertension.
- Without a known trigger, high pressure inside the skull is called idiopathic intracranial hypertension (IIH).
- If cerebrospinal fluid (CSF) builds up inside of the skull, a diagnosis of hydrocephalus is made.
- Diseases affecting the brain, like meningitis and encephalitis.
- Brain damage caused by trauma.
- Intracranial hemorrhage.
- Sinusitis and other infections that don’t go away for a long time.
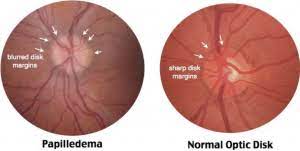
Risk Factors for Papilledema:
- Obesity: Obesity is a risk factor for papilledema because it can increase intracranial pressure.
- Age: Papilledema is more common in older adults.
- Gender: Papilledema is more common in women than in men.
- Family history: A family history of papilledema or intracranial hypertension increases the risk of developing this condition.
Malignant hypertension occurs when there is a sudden increase in blood pressure that puts the body’s organs at risk of damage. It often occurs in people with a history of high blood pressure. But it can also occur in people with normal blood pressure. The condition is a medical emergency that requires immediate attention.
Levels of Degree:
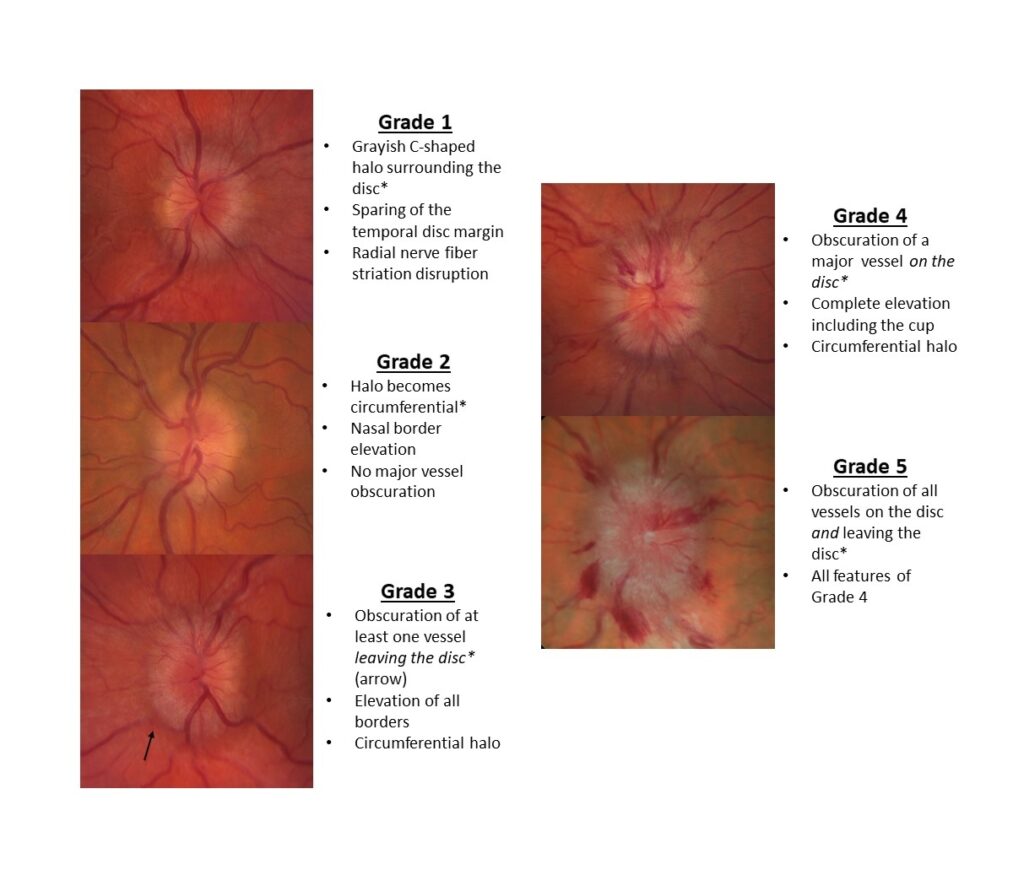
Papilledema is classified into four levels of severity, based on the degree of swelling of the optic disk. These levels are:
- Mild: The swelling is barely noticeable and there is no loss of vision.
- Moderate: The swelling is noticeable and there may be some vision loss.
- Severe: The swelling is pronounced and there is significant vision loss.
- Very severe: The swelling is extreme and there is complete vision loss.
Treatment of Papilledema:
The treatment of papilledema depends on the underlying cause. In most cases, treatment involves reducing intracranial pressure. This may involve:
- Medical Treatment: Medications such as acetazolamide or furosemide may be prescribed to reduce fluid buildup and intracranial pressure. Diuretics or corticosteroids may be prescribed to reduce fluid buildup and intracranial pressure.
- Tomography: CT or MRI imaging to rule out a space-occupying lesion. The optimal imaging modality is MRI and an accompanying contrast-enhanced MRV to rule out venous sinus thrombosis.
- Surgical Treatment: If a brain tumor is causing the papilledema, surgery may be necessary to remove the tumor.
- Lifestyle Changes: If obesity is contributing to the condition, weight loss may be recommended.
Symptoms of Papilledema:
- Blurred vision or double vision
- Visual field loss
- Headache
- Nausea or vomiting
- Fatigue
- Irritability
- Loss of peripheral vision